What is Kennedy's Disease
Kennedy's Disease goes by many names including Kennedy's Syndrome, Spinal Bulbar Muscular Atrophy, Spinal and Bulbar Muscular Atrophy, X-linked Spinal Bulbar Muscular Atrophy, X-linked Spinal and Bulbar Muscular Atrophy, and SBMA.
Kennedy's Disease is a rare X-linked recessive genetic progressive neuro-muscular disease. Both the spinal and bulbar neurons are affected causing muscle weakness and wasting (atrophy) throughout the body which is most noticeable in the extremities (legs/arms), it is especially noticeable in the face and throat, and causes speech and swallowing difficulties, major muscle cramps as well as other symptoms (please see the "Symptoms" section for more detail).
Kennedy's Disease is an adult-onset disease with symptoms usually appearing between the ages of 30 and 50. However, earlier and later onsets have been recorded. Life expectancy is noted to be at or almost normal.
Generally males with this inherited gene develop symptoms, while females with this gene are carriers. In rare cases, females have been known to exhibit symptoms as well.
It is estimated that 1 in 40,000 individuals worldwide have Kennedy's Disease. However, many go undiagnosed or misdiagnosed for years. The most frequent misdiagnosis is the fatal Lou Gehrig's Disease (ALS).
How is Kennedy's Disease diagnosed?
Fortunately, there is a simple blood test today that checks a person’s DNA for the defective chromosome. Almost any DNA testing laboratory can perform the test. A doctor or nurse can draw the blood and send it off to the laboratory. Test results are normally returned within three-to-six weeks. See DNA Testing and Labs for additional information on the actual DNA test and labs that can perform the test.
Common Misdiagnosis
Important: A DNA blood test can determine if Kennedy's disease is the correct diagnosis.
The most frequent misdiagnosis has been ALS (Lou Gehrig's Disease). Below are other diseases that share similar symptoms with Kennedy's Disease and have caused Kennedy's Disease patients to be misdiagnosed. .
The most common misdiagnoses that many individuals with Kennedy's Disease have received:
- Amyotrophic Lateral Sclerosis (also known as: ALS or Lou Gehrig's Disease)
- Spinal Muscular Atrophy III - Kugelberg-Welander
- Glycogen Storage Disease
- Guillain-Barre Syndrome
- Myasthenia Gravis
- Multiple Sclerosis
What causes the symptoms that are associated with Kennedy's Disease?
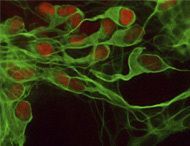
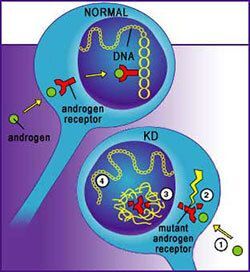
Motor neurons are long nerve cells that extend from your spinal cord to your muscles. These nerve cells fire to make your muscles contract. In KD (Kennedy's Disease) the nerve cells become dysfunctional and eventually die, leaving the muscles unable to contract.
The androgen receptor is a protein that resides inside the nerve cell. Many cells have the androgen receptor protein, but motor neurons have more than most. The binding of testosterone to an androgen receptor somehow causes the onset of the disease. Men are generally affected by KD because they have much higher levels of testosterone than women.
Is there a treatment or cure for Kennedy's Disease?
Unfortunately, there is no know treatment or cure, but researchers continue to make strides every year. Some individuals living with KD do take medications prescribed by their medical doctor to help alleviate various symptoms. Others have reported that a smart (light) exercise program coupled with stretching helps. If you have questions, visit the KDA Forum or contact the KDA.
How did Kennedy’s Disease get its name?
In 1964, George B. walked into the office of William R. Kennedy, MD. George was the first recognized person with Progressive Proximal Spinal and Bulbar Muscular Atrophy of late onset, a sex linked recessive trait. The identification of this condition in families by Dr. Kennedy was the beginning of the study that has grown to include medical researchers around the world attempting to find a cure for what is universally known today as Kennedy’s Disease.

